Abstract
As we approach a collective longevity milestone in the United States, we can take rapid action to plan for adapting our communities in ways that optimize the aging experience. Called Connected Communities, they are places where people of different ages and abilities live together, access support when needed, and remain connected to the social and economic life of their neighborhoods. Housing, healthcare, supportive services, workforce development, and civic life are intentionally woven together to form a community-driven continuum of support grounded in dignity, equity, and accountability. A pragmatic, detailed look at how to create such places.
Key Words
Connected Communities, Continuing Care Retirement, Village to Village Network, Presbyterian Villages, workforce
In turbulent times—when longstanding publicly funded healthcare coverage programs are downsizing and public health services are dwindling (and in some cases simply disappearing)—it is easy to lose sight of what we can do better, and what organizing things differently will accomplish.
In some ways, this is the best time in a generation for making changes at the local level. As we approach a collective longevity milestone in the United States, where by 2030 all of the more than 70 million Baby Boomers will be ages 65 and older, we can take rapid action to plan for adapting our communities in ways that optimize the aging experience (AARP, 2023; U.S. Census Bureau, 2023). This inherently positive exercise starts with thinking about ways to help people (and ourselves) continue to make personal connections and contributions. It calls for embedding shared services and supports at the neighborhood level to make ongoing relationships, choice, and autonomy possible for people of varying abilities. It prioritizes the preferences of those who receive supportive services, honors those who provide them, and joins the interests of sustainable economic development with the interests of a population benefiting from multi-ability, multi-generational neighborhood life. We call this framework of action “Connected Communities.”
The concept of Connected Communities has emerged from a growing recognition among innovators in aging, disability services, housing, and community development that the prevailing architecture of long-term care no longer aligns with the aspirations of a long-lived society. Rather than organizing support around age- and disability-segregated institutions or fragmented service systems, Connected Communities propose something simpler and more ambitious: places where people of different ages and abilities live together, access support when needed, and remain connected to the social and economic life of their neighborhoods. In this model, housing, health care, supportive services, workforce development, and civic life are intentionally woven together to form a community-driven continuum of support grounded in dignity, equity, and accountability.
The framework has been shaped through the collaborative work of leaders from across several sectors who for decades have been reimaging community life. Together with colleagues developing new models of shared housing, culture-change pioneers, disability advocates, direct care workforce champions, and sustainable community-development strategists have convened practitioners, researchers, and lived-experience leaders to explore a simple but transformative question: What if we assembled the expertise and proven practices already in the field to create a continuum of care that renders age- and disability-segregated institutions obsolete?
The resulting vision did not arise from theory alone. It reflects lessons drawn from real places where pieces of the model already exist: Green House homes and culture-change initiatives like The Eden Alternative, PACE programs, affordable housing developments, disability-led community living models, age-friendly ecosystems, and neighborhood revitalization projects such as the Thome Rivertown Neighborhood initiative in Detroit. These efforts demonstrate that when housing, services, and community life are intentionally aligned, the benefits extend beyond individual well-being to include workforce development, neighborhood revitalization, and broader economic impact.
In that sense, Connected Communities are best understood not as a single program, but as an evolution of models already working in practice. The framework uses appreciative inquiry to identify what is succeeding across the aging, disability, and housing ecosystems with a vision to knit those elements into locally designed continuums of support. These communities typically include affordable and mixed-income housing options, integrated health and supportive services, intergenerational and multi-ability living environments, accessible green spaces and community hubs, and workforce housing and training opportunities.
Building on What Works
Momentum for the concept is building. Across the United States, leaders are exploring how Connected Community principles can guide the design of new neighborhoods and the reinvention of existing care systems. The framework resonates because it aligns with multiple priorities: expanding accessible housing, integrating health and social services, strengthening the direct care workforce and enabling people to age and live with disability in places that remain connected to family and community life.
Connected Communities provide a shared language for efforts already underway in many regions, while encouraging new partnerships among sectors that historically worked in isolation. As these collaborations deepen, the initiative aims to accelerate momentum toward a future in which community-based continuums of support become the norm rather than the exception in how communities organize care and belonging in an era of longevity.
There are multiple examples of how Connected Communities can be ideated. For decades, “Life Plan” communities (originally known as Continuing Care Retirement Communities) have offered independent, assisted living, and skilled care to people who have the means to buy in, with the best of them serving as hubs for broader community life and connection.
The vibrant Village-to-Village Network (https://www.vtvnetwork.org/) uses volunteers to organize information on supports and social services for members living in a given area (and who pay a modest fee) to help one another age in community (Goff & Duran, 2024). Projects led by farsighted entrepreneurs mix private and public funding for those whose incomes are low, and who need housing and supportive services (Golant, 2022). Others are intergenerational—for example, Bridge Meadows (https://bridgemeadows.org/) in Oregon, and Carehaus in Chicago (https://www.carehaus.net/).
‘The initiative aims to accelerate momentum toward a future in which community-based continuums of support become the norm.’
There are initiatives led by long-established faith-based providers such as Presbyterian Villages of Michigan (PVM), which has built comfortable, accessible housing-with-services communities for lower-income older adults in areas of high socioeconomic need (https://www.pvm.org/). In the case of Thome Rivertown, PVM worked with the Henry Ford Health System, Brio Senior Living, and PACE Southeast Michigan on a successful 12-year-old project that braids together HUD 202 low-income senior independent housing, state-, and city-funded low-income housing with services, a PACE adult day health center, and clinic on the ground floor (Arku et al., 2022), two floors of Green House household model long-term services and supports (Zimmerman et al., 2016, 2021) (licensed as Michigan’s equivalent of assisted living), and nutrition services contracted through the local Area Agency on Aging.
There are visionary leaders in the Intellectual and Developmental Disabilities community such as Many Hands Lifesharing Community in Michigan (https://manyhandslc.org/home) who are creating housing-with-services initiatives for this growing population, their family members, and care partners. As aging trends accelerate, there will likely be a surge of interest among healthcare and housing providers to offer a range of supportive services, which must be flexible enough to evolve over time as individuals’ needs change (Fulmer et al., 2021).
If these organizations are willing to work in close coordination with community leaders and local experts and advocates, multiple Connected Communities can be created. Now is an excellent time to bust silos between aging and disability services programs by aligning around a common rallying point: access to affordable, community-integrated housing for all. Rather than gathering people in buildings and gated communities that are segregated by age, disability, and/or income, it is possible to design for a cross-section of people and to welcome all in the shared endeavor through a lens of asset-based community development.
National Map Graphic
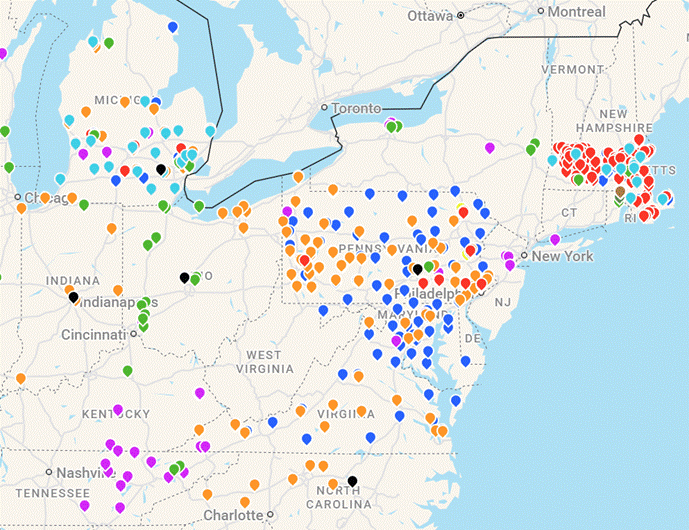

Mapping Connected Communities
Our experience engaging a range of leaders suggests there are many key partners who would likely be interested in participating in the design and building of a Connected Community. We have developed a work-in-progress interactive map that illustrates some of those partners, from Village-to-Village Network communities to Age-Friendly Community initiatives focused on social participation, intergenerational life, and new models to promote livability for all. The map’s legend displays a cross-section of potential partner organizations that can be invited to participate in collaborative discussions around virtual and actual tables.
Preconditions for a strong multi-sectoral partnership include interest and input from planning organizations, providers who are committed to the area and span a continuum of care (light-touch services, moderate care, and skilled care), housing organizations, community economic development experts, funders, and local leaders (e.g., the mayor, the county board, zoning boards, city planners, etc.)—all coming together give life to an Age-Friendly Ecosystem (Fulmer et al., 2023). Together with energetic advocates and volunteers, these parties can be formed into a steering committee to launch a project and plan steps to take it forward.
From Renderings to Reality
To spark enthusiasm and coalesce around a common vision, a rendering can be prepared to show what the local Connected Community would include. Figure 1, below, shows a rendering of a Connected Community in the pipeline in Rhode Island, which envisions a newly built neighborhood with cottages for people who need supportive services, workforce housing for those delivering the services, a building for medical providers, a park, and a social hub for those living adjacent and anyone else who wishes to come and participate in activities the community wants to sponsor and to host (e.g., yoga, theater, parties, book club discussions).
FIGURE 1
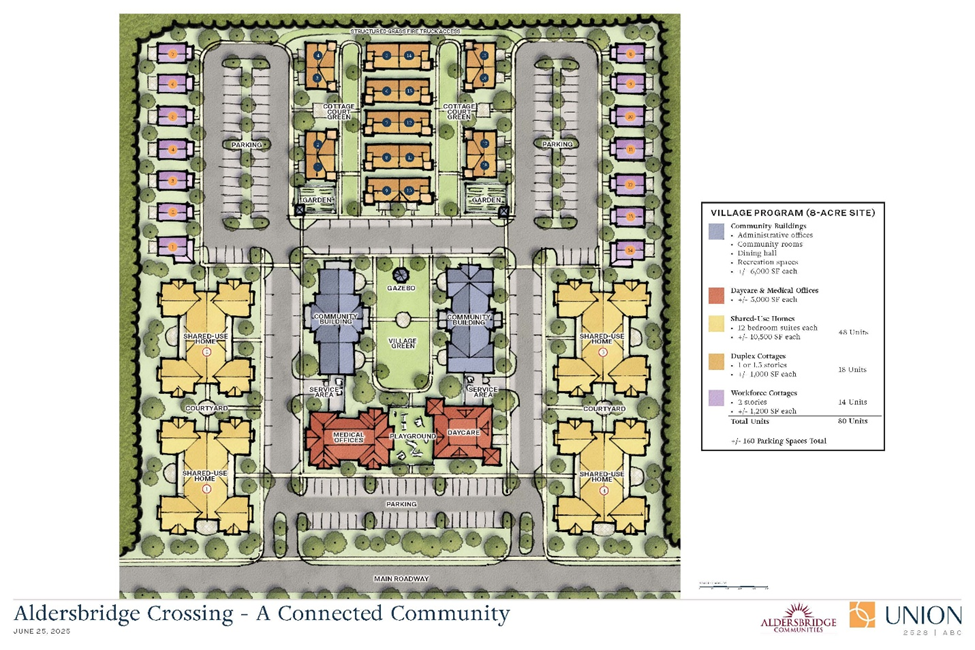
Different (likely more vertical) Connected Communities can be designed for dense urban areas that make innovative re-use of existing buildings. Other types of neighborhoods can be created within an existing college campus, a former mall or farm, and other areas that would benefit from redevelopment. The most successful projects are likely to be those informed by ongoing contributions from key individuals and organizations (inclusive of those named above) that commit to working in partnership to solve the financing requirements of a Connected Community; to establish guidance for an accountable and transparent management culture; to foster person-centeredness in supportive services delivery; to measure quality and satisfaction among those living and working in the neighborhood; and to oversee and publicly discuss financial operations and returns to investors, along with planned physical and operational improvements.
Financing Connected Communities
In the foundational area of financing, the primary sponsors and architects of a Connected Community can look to blended capital stacks, starting with tax-incentive programs that include Opportunity Zones, New Market Tax Credits, Low-Income Housing Tax Credits, Historic Preservation Tax Credits, Brownfield Tax Credits, and Energy Efficiency Tax Credits. The mix of financing also will include bank loans, philanthropy, and social-impact bond-investment models structured with long-term state budget implications in mind. Neighborhoods aiming to attract a robust mix of residents, including middle-class and higher-income individuals, may offer co-op and/or condominium housing arrangements, where housing equity can be grown as all boats rise and rates of Medicaid spend-down are slowed.
Ongoing operational funding derives from health programs financed by Medicare, Medicaid, the Older Americans Act, and other programs for which older adults and individuals with disabilities are eligible, as well as out-of-pocket funding from beneficiaries (Crowley et al., 2022). Projecting income from publicly financed programs that subsidize rents for lower-income populations is key, as is funding from other programs supporting people living in a given Connected Community (e.g., those administered by the Dept. of Veterans Affairs).
Prioritizing Workforce
A Connected Community cannot develop without deliberate investment in a stable, well-educated direct-care workforce. The shortage of direct-care professionals is structural, not cyclical (PHI, 2023). Vacancy rates across nursing homes, assisted living, and home care settings remain high, wages are stagnant, and immigration constraints further destabilize a workforce long sustained by newcomers (Scales, 2021). Contributors to Generations have repeatedly underscored this fragility. An age-friendly future cannot rest on precarious labor systems. Without workforce justice, age-friendly reform will remain rhetorical (Harootunian et al., 2023).
‘Different (likely more vertical) Connected Communities can be designed for dense urban areas that make innovative re-use of existing buildings.’
Connected Communities can respond by embedding workforce education within neighborhood design. Rather than treating training as episodic compliance delivered by fragmented employers, Connected Communities function as place-based workforce academies. Education is continuous and visible. Didactic instruction, apprenticeship, interdisciplinary team review, and mentorship are woven into communal life. Fortunately, robust training protocols have already been framed out that can be assembled into modules featuring relationship competencies: advocacy, communication, conflict resolution, cultural competency, leadership, problem-solving, professionalism and ethics, teamwork and collaboration, and time management and accountability. The following general competencies would also be covered: in Activities of Daily Living, health and wellness transitions of care, age-related changes, detection of individual changes in condition, crisis prevention and intervention, abuse, infection control and prevention, pain management, safety, end of life care, and quality assurance.
Connected Communities operationalize the Age-Friendly Ecosystem framework advanced in Generations Journal (Spring 2025, “The Promise of an Age-Friendly Ecosystem”), which called for alignment across housing, health systems, public health, business, and higher education (Phillips et al., 2025). At the neighborhood scale, housing-with-services becomes workforce infrastructure. Community economic development becomes talent strategy. Civic planning is a public health endeavor that takes seriously the demographic realities in communities where a shared awareness that “we’re all aging” becomes common cause for an inclusive, lifespan developmental approach to well-being, where childcare options are designed into the fabric of the community to promote intergenerational life and make employment in the Connected Community attractive.
The economic framing of a Connected Community is rooted in health equity concerns outlined in Generations Journal (Summer 2021, “Precarious Aging and Late-Life Poverty”) where demographic aging is approached as a market-shaping transformation rather than a fiscal burden—and where health-equity issues center increased funding in social investments and social services with closer collaboration between social and medical care systems (Robert & Morales, 2021). Connected Communities translate abstractions into physical form: mixed-income housing, co-located services, and structured career ladders generate both care capacity and local economic resilience.
Our current workforce instability disproportionately harms low-income communities and communities of color (Dill & Duffy, 2022). Part of the solution is embedding competency development in daily communal practice, which works to reduce service fragmentation, and elevate direct care professionals to be civic contributors rather than invisible labor. Within Connected Communities, direct care competencies are reinforced through lived experience, while role clarity and person-centered practice are strengthened by proximity to interdisciplinary teams, reflecting cross-sector coordination.
Cultural competency and conflict resolution are cultivated through daily interaction in intentionally diverse, multigenerational environments that advance equity principles. Leadership and quality improvement are elevated when workforce members participate in listening sessions, surveys, meetings, quality dashboards, and broader community forums, thus positioning aging reform within civic infrastructure and sound governance. Further, co-location of housing, primary care, behavioral health, and supportive services can be leveraged to reinforce competencies in transitions of care, infection control, chronic condition management, and social determinants of health. Lifelong learning can readily be operationalized and made normative through partnerships with community colleges and workforce boards that create stackable credentials and portable career pathways.
As workforce development is embedded in the built and social architecture of Connected Communities, the conceptual framework of an Age-Friendly Ecosystem becomes an operating reality. Housing-with-services is no longer a programmatic afterthought, but rather a deliberate strategy for local economic growth and capital formation. Investment in direct care professionals is not only labor support, it is part and parcel of neighborhood stabilization policy that is grounded in demographic fact. In a society now being rapidly reshaped by longevity, care work must be recognized and structured as essential civic infrastructure—skilled, visible, and integral to the long-term vitality of communities.
Policymakers can do much to help with funding and championing Connected Community neighborhoods in the areas and states they represent.
Policymakers can do much to help with funding and championing Connected Community neighborhoods in the areas and states they represent. Grounded in the practical logic of community economic development and supported by positive aging innovators in long-term services and supports like AgingIN and The Eden Alternative, as well as consumer advocates like the Gray Panthers NYC and the Live Oak Project, policymakers can help to bring recognition to a movement of down-to-earth civic reforms. Collectively, we can support one another to work on an ongoing basis with local, regional, state, and federal officials to incentivize inclusive planning, blended financing, and cross-sector governance (Greenfield et al., 2022). Old age does not have to be about impoverishment and suffering.
Notably, the extremely low incomes required by Medicaid for long-term services and supports (LTSS) can and should be tempered with thoughtful policy that incentivizes individuals to save for current and future needs—without being stripped of access to needed services. And many who have amassed some equity (in the form of a modest house, for example) could be incentivized to leverage that equity for accessible housing-with-services arrangements as their needs change.
Age-Friendly leaders can move beyond producing reports to capital development, and work to encourage and sponsor partnerships between aging and disability advocates and community-minded housing developers (Hong et al., 2023). Philanthropy and impact investors can provide seed funding and technical assistance for getting Connected Community–style projects up and running. In the process, they should embrace blended-return frameworks that include social Returns on Investment (ROI) and aggregated precision investment (Nielsen et al., 2021). Investors of all stripes can ask communities what they want and need in the form of residential and commercial development to build a solid, sustainable infrastructure for delivering supportive services.
Finally, as community members with lived experience in our own neighborhoods, we can all draw on lessons to be harvested from places like the Netherlands, where mutual aid policies are clearly woven into benefit design (Veghte, 2025). And we can learn from examples in one of the oldest societies in the world, Japan, where asset-based community development approaches such as Ibasho build on the wisdom of elders to guide the future (Kiyota et al., 2024).
Conclusion
By organizing and sponsoring ongoing meetings and collaborative discussions organically where we live, all of us are poised to contribute to meeting this moment: We can collaborate to make rapid, replicable changes and adaptations that fit the purpose of a long-lived society, and galvanize the planning and design processes necessary for standing up Connected Communities. As this framework continues to gain traction among innovative practitioners and responsive policymakers, now is the time to reimagine longevity, not as a burden to manage, but as an opportunity to strengthen the social and economic foundations of our neighborhoods. And to do so in communities where bonds may be frayed but not broken—where relationships matter, and hope is our common currency. Let’s get to it!
Anne Montgomery, MS, is an experienced policy analyst and health systems researcher specializing in long-term care and support systems for older adults and individuals living with disabilities. An independent consultant working with the National Committee to Preserve Social Security and Medicare, AgingIN, the Live Oak Project, and Gray Panthers NYC, Montgomery served the U.S. Congress for a decade, developing legislative policy for the Senate Special Committee on Aging and the House Ways & Means Committee. She also served as Altarum’s director of the Center for Eldercare and Advanced Illness.
Joe Angelelli, PhD, is the CEO of Lifespan, Inc., in Homestead, PA, and serves on ASA’s Generations Journal Editorial Advisory Board. Lifespan is a nonprofit agency providing critical support and services for residents ages 60 and older in Allegheny County, Penn. Angelelli has more than 25 years of experience in thought leadership, systems transformation, and community partnerships.
Photo credit: Shutterstock/Juan Aizpuru
References
AARP. (2023). Global longevity economy outlook: the economic contribution of people age 50 and older. global-longevity-economy-report.doi.10.26419-2Fint.00052.001.pdf
Arku, D., Felix, M., Warholak, T. L., & Axon, D. R. (2022). Program of All-Inclusive Care for the Elderly (PACE) versus other programs: A scoping review of health outcomes. Geriatrics, 7(1), 31. https://doi.org/10.3390/geriatrics7020031
Crowley, R., Daniel, H., Cooney, T. G., & Engel, L. S. (2022). Long-term services and supports for older adults: A position paper from the American College of Physicians. Annals of Internal Medicine, 175(7), 1016–1022. https://doi.org/10.7326/M22-0864
Dill, J. S., & Duffy, M. (2022). Structural racism and Black women’s employment in the U.S. health care sector. Health Affairs, 41(2), 265–272. https://doi.org/10.1377/hlthaff.2021.01400
Fulmer, T., Reuben, D. B., Auerbach, J., Fick, D. M., Galambos, C., & Johnson, K. S. (2021). Actualizing better health and health care for older adults. Health Affairs, 40(2), 219–225. https://doi.org/10.1377/hlthaff.2020.01470
Fulmer, T., Dash, K., Shue, J., Chang, J., Huang, J., & Maglich, A. (2023). Age-friendly ecosystems: Expert voices from the field. Geriatrics, 8(4), 68. https://doi.org/10.3390/geriatrics8040068
Goff, M., & Doran, P. (2024). Co-producing age-friendly community interventions: The village model. In Reimagining age-friendly communities (pp. 118–134). Emerald Publishing.
Golant, S. M. (2022). Housing America’s older adults: Meeting the needs of an aging population. Journal of Aging & Social Policy, 34(4–5), 569–586.
Greenfield, E. A., Oberlink, M., Scharlach, A. E., Neal, M. B., & Stafford, P. B. (2015). Age-friendly community initiatives: Conceptual issues and key questions. The Gerontologist, 55(2), 191–198. https://doi.org/10.1093/geront/gnv005
Harootunian, L., Buffett, A., O’Gara, B., Perry, K., Werber Serafini, M., & Hoagland, G. W. (2023, June 13). A multipronged approach to alleviating the direct care workforce shortage. Health Affairs Forefront. https://doi.org/10.1377/forefront.20230608.815571
Hong, A., Welch-Stockton, J., Kim, J. Y., Canham, S. L., Greer, V., & Sorweid, M. (2023). Age-friendly community interventions for health and social outcomes: A scoping review. International Journal of Environmental Research and Public Health, 20(3), 2554. https://doi.org/10.3390/ijerph20032554
Kiyota, E., Nishita, C., Tanaka, Yl, Ah Sue, E., & Turner, H. (2024). The Ibasho model of elder empowerment and community ownership. Generations Journal, 48(1), 1–6.
Many Hands Lifesharing Community. (n.d.). https://manyhandslc.org/home
Nielsen, R., Muhlestein, D., & Leavitt, M. O. (2021). Social determinants of health: Aggregated precision investment. Health Affairs Forefront. https://doi.org/10.1377/forefront.20210610.92852
PHI. (2023). Direct care workers in the United States: Key facts. PHI National. https://phinational.org/resource/direct-care-workers-in-the-united-states-key-facts
Phillips, K., Wolfe, M., & Shue, J. (2025). Creating a harmonious age-friendly ecosystem that delivers: Where do we go from here? Generations. https://generations.asaging.org/creating-age-friendly-ecosystem-delivers/
Robert, S. A., & Morales, M. J. (2021). Addressing health equity for older adults at the neighborhood level. Generations, 45(2), 1–11.
Scales, K. (2021). It is time to resolve the direct care workforce crisis in long-term care. The Gerontologist, 61(4), 497–504. https://doi.org/10.1093/geront/gnaa116
U.S. Census Bureau. (2023). 2023 national population projections tables. U.S. Department of Commerce. https://www.census.gov/data/tables/2023/demo/popproj/2023-summary-tables.html
Veghte, B. W. (2025). Promising policy innovations to make aging in the community affordable for all: Lessons from the Netherlands. National Academy of Social Insurance. https://www.nasi.org/wp-content/uploads/2025/01/Promising-Dutch-Long-Term-Care-Innovations.pdf
Zimmerman, S., Bowers, B. J., Cohen, L. W., Grabowski, D. C., Horn, S. D., Kemper, P., & THRIVE Research Collaborative. (2016). New evidence on the green house model of nursing home care: Synthesis of findings and implications for policy, practice, and research. Health Services Research, 51(Suppl 1), 475–496. https://doi.org/10.1111/1475-6773.12430
Zimmerman, S., Dumond-Smith, M., Tandan, M., Preisser, J. S., Wretman, C. J., & Sloane, P. D. (2021). Nontraditional small house nursing homes have fewer COVID-19 cases and deaths. Journal of the American Medical Directors Association, 22(3), 489–493. https://doi.org/10.1016/j.jamda.2021.01.024












