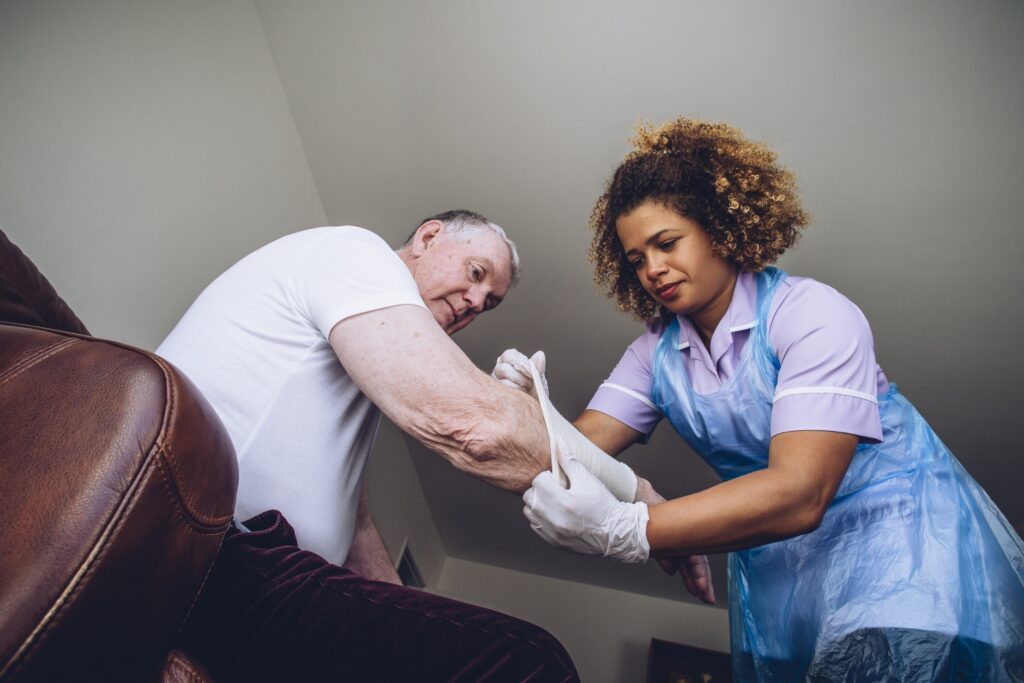
The concept of nursing homes has always been off-putting to some, and the global pandemic certainly hasn’t altered that opinion in a positive direction. However, nursing homes differ widely and many are striving not only to keep their residents safe, but also to provide better preventive care during the pandemic.
One focus that recently surfaced is promoting better mouth care in nursing homes, by training all staff and having a direct care worker specifically to attend to the care of residents who require more time, and fill in as needed when staff is stretched thin. It’s even more important in in the time of COVID-19 because dentists are no longer regularly visiting nursing homes as some had been prior to the pandemic.
The concept that oral healthcare is preventive healthcare is backed by research from Sheryl Zimmerman, Philip Sloane, Kimberly Ward and colleagues in a paper published in JAMA Network Open, “Effectiveness of a Mouth Care Program Provided by Nursing Home Staff vs Standard Care on Reducing Pneumonia Incidence: A Cluster Randomized Trial.”
Generations Today recently spoke with study author Sheryl Zimmerman, University Kenan Distinguished Professor, School of Social Work, and co-director of the Program on Aging, Disability, and Long-Term Care, Cecil G. Sheps Center for Health Services Research, University of North Carolina at Chapel Hill, and staff development coordinator Patty Van Dyke, who implemented the program at Glenaire, a continuing care retirement community with a nursing home component in Cary, North Carolina.
The study analyzed the effects of using a program called Mouthcare Without a Battle with nursing home residents to prevent pneumonia. Remarkably, during the first year of the two-year study, pneumonia incidence was reduced by 31 percent among nursing home residents. By year two this number returned to the point of being statistically negligible, but researchers and Van Dyke say this is due to a return to status quo, staff habits and a turnover in staff, some of whom had not been trained in the program.
Zimmerman and colleagues developed Mouthcare Without a Battle (MCWB) after the success of a similar program called Bathing Without a Battle. Both programs help nursing home staff to more effectively and with less disruption aid people with Alzheimer’s in bathing and tending to their oral health.
The connection between oral health and pneumonia is a clear one, in that residents who have swallowing problems and other issues with their mouth and tongue often end up aspirating their food and other dislodged particles into their lungs. Generally in nursing homes, older adults’ mouths are “caked with plaque and gingivitis,” said Zimmerman. So they are likely aspirating bacteria along with food, leading to pneumonia. The majority of nursing home residents don’t receive needed help with mouth care, and at best, the average time spent conducting oral care can be as little as 15 seconds per day, said Zimmerman.
Ideally, older adults should brush and clean between teeth at least once per day.
Oral Health Care Without the Fighting
People living with dementia pose a particular challenge because they may not understand why someone is trying to help brush their teeth, and they may have mouth pain due to tooth decay or gum inflammation. As a result, they tend to fight staff who attempt to brush their teeth. The MCWB program, which was developed with funding from the Alzheimer’s Association and the Centers for Medicare & Medicaid Services (CMS), uses multiple methods to encourage people with Alzheimer’s to allow staff to perform mouth care, including friendly and persistent persuasion, brushing at night when residents are drowsy and less resistant, having an extra toothbrush if a person living with dementia clamps down on one (a natural response to something being put in their mouths), and even singing, as the staff member can gently put a toothbrush into their open mouth as they sing.
Van Dyke found the most effective tool to be the personality of Tremaine, the trained oral care aide they used during the study. Some residents who live with dementia became so positively conditioned to Tremaine’s way of tending to their teeth that they would open their mouths as soon as she entered their rooms. The trust and specific MCWB techniques promoted the acceptance of Tremaine providing mouth care to her residents.
A definite reduction was seen in pneumonia cases, due to people’s mouths having less bacteria. Van Dyke feels that renewed training in MCWB would be beneficial to prevent staff from falling back on old habits. She continues to push for the return of Tremaine, at least part-time, to work with residents and staff to prevent infections.
The benefits of MCWB and oral health aides are not limited to preventing pneumonia, however, as Zimmerman says such programming—which she gives away at no cost to anyone who wants it, including family caregivers—has the likely added benefit of saving Medicare money as it prevents the numerous hospitalizations associated with pneumonia. The program is available at Mouthcarewithoutabattle.org.