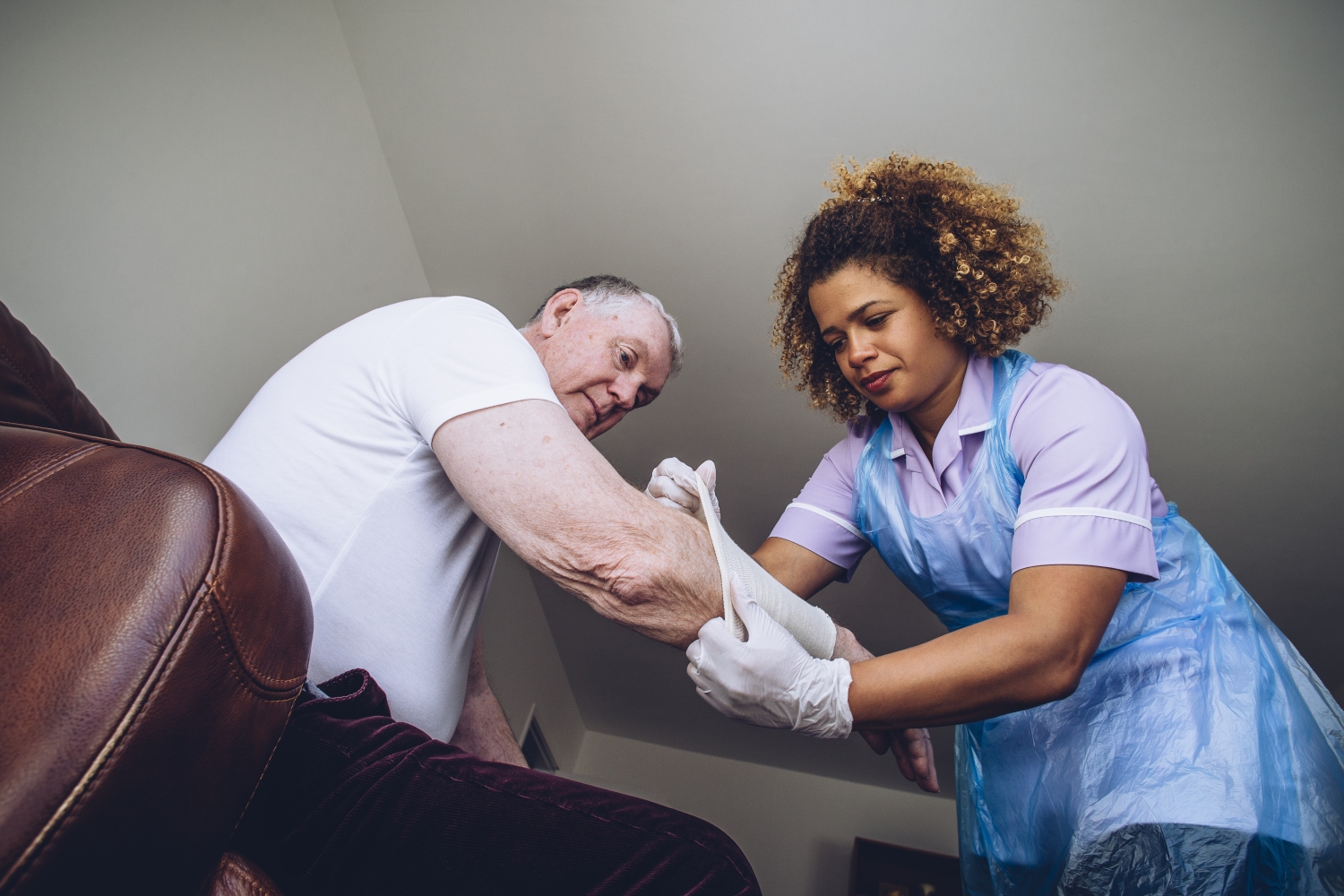
Chronic wound rates among older adults are rising, impacting an estimated 10.5 million of U.S. Medicare beneficiaries. Chronic non-healing wounds can significantly increase healthcare costs and exact a substantial human toll, impacting health outcomes and the quality of life of patients and their families.
As advanced practice providers working in mobile wound management, we have seen firsthand how bringing expert treatment directly to patients’ homes transforms lives—especially for older adults and those with limited mobility. Our goal is to meet patients where they are, delivering high-quality wound management that not only accelerates healing but also restores their personal sense of well-being. In this post we outline opportunities to improve wound healing outcomes through a mobile wound management model and its standardized protocols, including critical components like quality nutrition care.
The Rise of Mobile Wound Management
Mobile wound management is growing rapidly, driven by an aging population, increasing rates of chronic conditions like diabetes and obesity, and evolving Medicare payment models that reward quality care delivered at home. Importantly, advances in wound imaging have made it easier than ever to bring specialized care directly to the patient’s doorstep.
For many older adults and people living with mobility challenges, leaving home for repeated wound clinic visits can be stressful, exhausting or even unsafe. By providing care where patients feel most comfortable, at home, we reduce the risks of infection and hospitalization, while honoring their dignity and independence. In addition, we help ease patients’ financial burden by reducing common out-of-pocket costs, such as travel expenses and co-pays. This approach helps relieve the burden on caregivers, too, giving families peace of mind that their loved one is receiving expert, compassionate treatment without unnecessary travel.
Wounds usually progress through normal stages of healing to close within about a month; beyond that they are considered chronic wounds. The chronic wounds we most frequently encounter at home include: diabetic foot ulcers, venous and arterial leg ulcers, pressure injuries, trauma and surgical wounds, which can be more advanced than those treated in primary care clinic settings. This is because the wounds are often complicated by comorbidities, delayed treatment, poor nutrition and/or limited mobility, all of which makes specialized, consistent care essential.
Mobile wound care fosters a shorter healing time—with patients’ wounds healing on average nearly twice as fast.
Further, unlike more general home health agencies which are primarily focused on overall patient care and support, our care teams bring advanced training, tools and treatments to specifically care for patients’ wounds. The specialized care we provide can include sharp debridement, ordering labs and diagnostic studies, performing biopsies, and adjunctive therapies such as negative pressure wound therapy, among others. This ensures that patients receive the highest level of care in the comfort and safety of their homes and importantly leads to improved health outcomes and reduced costs compared to traditional, clinic-based treatment (see box below).
A Mobile Wound Medicine Model Specifically Focused on Healing the Wound
Our focus is on healing wounds, not just treating them. To achieve this our mobile wound management model has five core components:
- Advanced treatment techniques based on an understanding of chronic, non-healing wounds and their root causes;
- Comprehensive care plans personalized to reflect each individual patient’s medical history, wound type and progression, and underlying conditions that can impact healing;
- Preventing downstream complications by identifying early signs of complications, managing risks, and intervening promptly to prevent the need for more costly and invasive treatments;
- Patient education and support to empower patients and caregivers and ensure long-term success and higher quality of life;
- Faster, more efficient healing supported by proprietary technology and onsite care that expedites the treatment process.
The underlying care principles and benefits of our mobile wound model are outlined below.
Care Principles and Benefits of the Mobile Wound Management Model
| Care Principle | Benefit |
| When care comes to the patient, it is easier to stay consistent with treatment. | Patients are more engaged when they feel safe and supported in their own environment, and caregivers can participate more fully in daily wound management. Clinicians can refer patients (even those not currently receiving homecare) directly to mobile wound management at any time and patients can also self-refer. |
| Partnering with the patient builds trust, improves adherence, and leads to stronger healing outcomes. | Concierge wound medicine providers meet patients wherever they are in the wound-healing process and patients do not need to be specifically homebound to receive concierge wound management. |
| Home-based care reduces stress. | Arranging transportation, missing work, or even managing multiple appointments can be stressful for patients and caregivers. Emotionally, patients often feel calmer and more respected when care is delivered in familiar surroundings. For caregivers, this reduces anxiety and helps them feel supported rather than overwhelmed. |
| Healing is strongest when care is coordinated. | Wound management providers document home visits in real time, communicate regularly with referring clinicians, and share clear treatment plans with home health teams. Primary care providers receive each visit note once complete. This ensures every member of the care team is on the same page, supporting the patient consistently and safely. |
| Direct-line communications with experienced care leaders benefit front-line care providers and patients. | In our model, we have an Infectious Disease specialist. This means our providers have direct access to infectious disease consultations, eliminating treatment delays, ensuring timely clinical decision-making, and strengthening patient outcomes by integrating a collaborative approach into our mobile in-home wound management model. |
High-quality wound medicine means more than changing dressings. Our mobile wound management model uses a multidisciplinary approach, as needed, to ensure accurate diagnosis, thorough wound assessment, infection control, debridement, moisture balance, offloading DME (durable medical equipment), which uses devices to relieve pressure on a wound, vascular screening, nutrition support, ongoing patient education, and holistically addressing social determinants of health. We integrate all of these factors into home visits, tailoring care to each patient’s unique needs.
Nutrition: The Unsung Hero of Mobile Wound Healing
Nutrition is often overlooked in wound medicine, yet it is foundational to wound healing and remains a powerful tool for mobile wound management. Without adequate protein, hydration and key nutrients like vitamin C, E, B12, calcium, and zinc, the body cannot repair tissue effectively. Older adults are especially vulnerable to malnutrition, which can slow healing and increase the risk of complications.
For our patients, we assess nutrition status at the start of care and every 90 days, screening for weight changes, appetite, hydration, and protein intake. We also use the Braden Scale monthly to monitor nutrition-related risk factors. What sets our approach apart is its practicality; during home visits, we look inside patients’ pantries and refrigerators to understand real-world dietary habits and barriers. This allows us to offer tailored guidance, recommend specialized nutrition supplements, and refer patients to dietitians when needed.
‘Nutrition is often overlooked in wound care, yet it is foundational to wound healing and remains a powerful tool for mobile wound care.’
Education is key to empowering patients and caregivers to play an active role in role in recovery. For nutrition, we talk about important nutrients, hydration goals, and meal planning as well as explain why their nutrition choices matter. Through clear, simple conversations and tangible materials/handouts we explain the importance of:
- Protein—the building block for new tissue
- Hydration—important to transport nutrients to the wound
- Specialized nutrition products—high protein oral nutrition supplements can help patients meet their protein needs when they cannot consume enough protein through diet alone. Nutrition supplements designed to support wound healing are also beneficial. These are science-backed formulations containing critical nutrients such as arginine, glutamine, HMB (beta-hydroxy-beta-methylbutyrate), collagen peptides and micronutrients.
Looking Ahead at Further Innovations and Opportunities in Mobile Wound Management
Advancements in technology and therapies, monitoring apps and devices, and availability of telehealth supported the development of mobile wound management as a safe, viable, and high-quality care option. The future of mobile wound management is being shaped by new research and developments that will make wound healing even more accessible, personalized and efficient for patients in their homes.
We partner with mobile lab and diagnostic companies to perform baseline testing in the home, eliminating the need for travel and delays in treatment. Additionally, we utilize a lab that employs DNA-PCR testing for cultures, which provides expedient and accurate results for the best patient outcome.
To continue to improve quality of care and outcomes for older adults, we recommend:
- Prioritize early identification and proactive wound prevention, including routine risk assessments, nutrition screening, and education for patients and caregivers to reduce avoidable complications.
- Strengthen clinical integration across the care continuum, ensuring seamless communication between providers, home health, specialists, and payors so patients receive timely, coordinated interventions.
- Invest in evidence-based training and ongoing competency development, equipping clinicians with the latest wound management techniques, technologies, and Medicare-aligned documentation standards.
- Leverage innovative diagnostics and point-of-care tools, such as mobile labs, DNA-PCR testing, and digital platforms, to accelerate accurate diagnoses and guide individualized treatment plans.
- Support whole-person care by addressing barriers beyond the wound, including mobility challenges, social determinants of health, caregiver strain, and access to essential supplies—empowering older adults to heal safely at home.
Together, these steps can ensure that patients and families not only receive expert care at home but also have the knowledge and support they need to feel confident throughout the wound healing process.
Natalie Kahle, MSN, APRN, FNP-C, DAPWHc, CWHAP, is a family nurse practitioner, wound specialist, and a national executive director for clinical integration and education for Woundtech. Desiree Lacandola, MSN, AAPRN, ANP-C, COCN, DAPWHc, is an adult nurse practitioner, wound specialist, and a national executive director of education and integration for Woundtech.
Photo credit: DGLimages